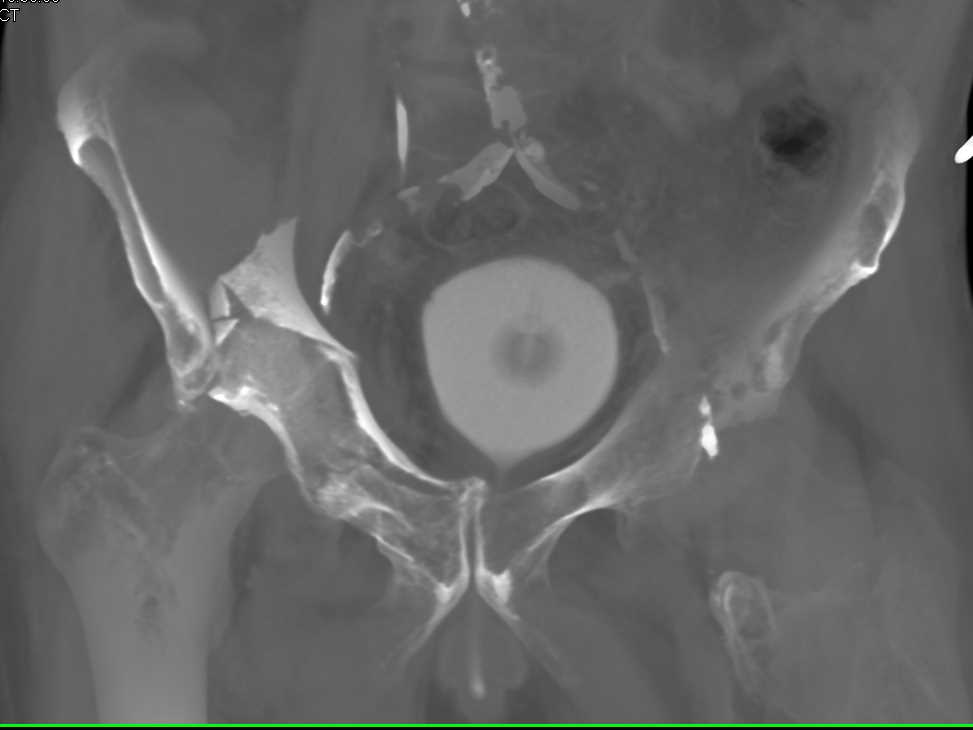
Even so, whenever possible, the surgeon tries to save the joint by doing an ORIF first. Of course, going right to a joint replacement surgery usually eliminates the need for a second surgery. The surgeon evaluates the best way to reduce blood loss, minimize operative times, and prevent complications. The decision is made on a case-by-case (individual) basis. In some cases, it's clear that the patient should have a hip replacement right from the start. If the patient is not a good candidate for ORIF (or if the ORIF procedure fails), then a total hip replacement may be the next step. The more bone fragments and the farther apart the bone fragments separate, the poorer the prognosis. The more closely the hip is restored to its normal shape and configuration, the better the results will be. The surgeon makes an incision to open up the hip, lines everything back up as much as possible, and uses plates, screws, pins, and/or wires to hold it all together until it heals. A procedure called open reduction and internal fixation (ORIF) pretty much describes what happens. The goals of treatment for all acetabular fractures are four-fold: 1) restore the weight-bearing surface of the socket, 2) keep good bone stock (strength and density), 3) maintain joint stability, and 4) prevent deformities.įor those patients who will have to have surgery, there are several options. Instead (with or without surgery), patients are encouraged to get up and move as early as possible. But this is no longer recommended due to the many complications that arise with immobility in this age group (e.g., blood clots, bed sores, pneumonia, deconditioning). Bedrest (even for displaced fractures) with tracton was once prescribed. But only minimal weight through the hip is allowed until healing occurs.Ī physiotherapist helps move the hip through its motions but with some limitations to protect it. So long as the fracture isn't displaced (shifted), those patients who could walk before the injury are allowed to walk with the support of a walker. The presence of dementia, poor health, severe bone loss, and nonambulatory status before the fracture are reasons why surgery may not be possible. And many times, this is still the most appropriate treatment. Until recently, this type of fracture was always treated conservatively (without surgery). Women tend to develop a break in the neck of the femur - long before there is any force up into the socket. Their femoral bones are thicker, stronger, and transfer a greater destructive force into the acetabulum. Older men are affected more often than women by this type of damage. That type of break is called a comminuted fracture. When that happens, there can be a single break or fracture line but more often the acetabular bone breaks into many tiny pieces. The reason it breaks is because the person falls (and lands) in such a way that the head of the femur (thigh bone) is driven up into the hip socket (acetabulum) with enough force to break bone. It is made of cartilage over bone just like every other joint. What's an acetabular fracture? The acetabulum is the socket side of the hip joint. Increasing age combined with certain risk factors such as osteoporosis (decreased bone density) makes it more and more likely that an older adult will end up in the hospital with an acetabular fracture.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
